Which antibiotics most commonly cause C diff?

James Craig
Published Jan 15, 2026
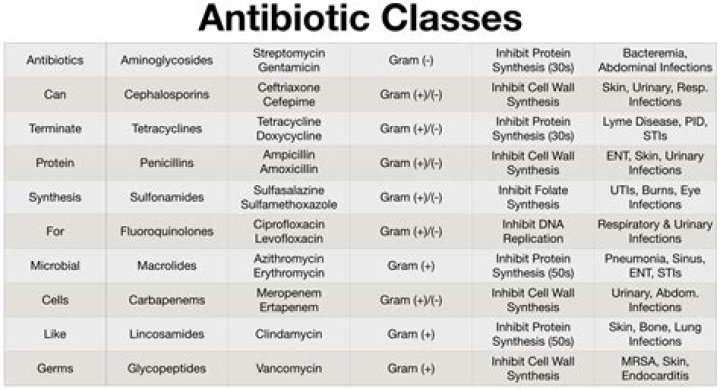
The primary risk factor for C difficile colitis is previous exposure to antibiotics; the most commonly implicated agents include the cephalosporins (especially second and third generation), the fluoroquinolones, ampicillin/amoxicillin, and clindamycin.
Which antibiotic is associated with the highest risk of C. difficile?
The results of the 3 meta-analyses are similar. Slimings and Riley (2014) concluded that cephalosporins and clindamycin are the antibiotics most strongly associated with hospital-associated C. difficile infection.
Which antibiotics have lowest risk of C. diff?
Which antibiotics are less likely to cause C. Diff?
- azithromycin (Zithromax, Z-Pak)
- clarithromycin (Biaxin)
- doxycycline (Oracea, Vibramycin)
- erythromycin (Eryped)
- fidaxomicin (Dificid)
- minocycline (Minocin, Solodyn)
- metronidazole (Flagyl)
How do you prevent C. diff when taking antibiotics?
Use of certain antibiotics, such as clindamycin and fluoroquinolones, is also linked to C. difficile infections. The best way to avoid infection with C. difficile is to take antibiotics as prescribed by your doctor and never share the medication with others.
Is C. diff common with antibiotics?
C. diff bacteria are commonly found in the environment, but most cases of C. diff occur while you're taking antibiotics or not long after you've finished taking antibiotics. People are 7 to 10 times more likely to get C.
21 related questions foundDoes Cipro Cause C. diff?
But, quinolones are more likely to cause C. diff than other antibiotics. Fluoroquinolones include popular drugs like levofloxacin (Levaquin), ciprofloxacin (Cipro), and moxifloxacin (Avelox), commonly used to treat bacterial sinusitis, urinary tract infections, and community-acquired pneumonia.
Can Cipro treat C. diff?
difficile were 'treated' with ciprofloxacin and clindamycin in a test-tube, and the growth of C. difficile monitored. The clindamycin-treated emulsions supported growth of C. difficile, while the ciprofloxacin-treated and control emulsions did not differ significantly and failed to support the growth of C.
What is the best antibiotic to treat C. diff?
Vancomycin and fidaxomicin are the most effective antibiotics against Clostridium difficile infections. They are both equally effective at wiping out an initial infection. However, patients treated with fidaxomicin have a lower rate of a recurrent C.
What's the best probiotic for C. diff?
The best studied probiotic agents in CDI are Saccharomyces boulardii, Lactobacillus GG (LGG) and other lactobacilli, and probiotic mixtures.
What color is C. diff poop?
Greenish stools were more common among the control cases. Another study correlated nurses' response as to whether a stool was positive or not for C. difficile based on stool odor.
Does doxycycline treat C. diff?
Doxycycline might directly inhibit C difficile, and small studies have shown that a similar agent (tigecycline) could be efficacious in treating C difficile infection. Doxycycline might also produce less disruption of enteric flora than other antimicrobials such as fluoroquinolones or carbapenems.
Does doxycycline cause C. diff?
Background: Receipt of antibiotics is a major risk factor for Clostridium difficile infection (CDI). Doxycycline has been associated with a lower risk for CDI than other antibiotics.
What's the safest antibiotic?
Penicillins are the oldest of the antibiotics and are generally safe (but they can cause side effects such as diarrhea, skin rash, fever and more). FQs are the newest group of antibiotics.
Can Pivmecillinam cause C. diff?
Pivmecillinam is well tolerated with a low side-effect profile. Pivmecillinam also has a minimal effect on the intestinal and vaginal flora of the host; thus, there is a lower rate of selection of resistant bacteria, vaginal candidiasis and, of note, Clostridium difficile.
Can Augmentin cause C. diff?
Nearly any antibiotic that disrupts the normal bowel flora may result in C. difficile infection and disease. Several antibiotics, however, are more commonly implicated: amoxicillin, amoxicillin-clavulanate (Augmentin, GlaxoSmithKline), second- and third-generation cephalosporins, and clindamycin.
What are the 4 C antibiotics?
Initiated in 2008, an early priority of the Scottish Management of Antimicrobial Resistance Action Plan was to reduce community and hospital use of antibiotics associated with C difficile infection, known as the 4Cs (ciprofloxacin/fluoroquinolones, co-amoxiclav, clindamycin, and cephalosporins).
Is yogurt good for C. diff?
Probiotics: Probiotics are friendly, live bacteria you need to combat the C. diff germ. They can be found in active yogurt cultures and in fermented foods, such as sauerkraut and miso. Probiotics help to reduce or eliminate watery diarrhea by putting good bacteria back into the gastrointestinal tract.
Can you get rid of C. diff completely?
People with Clostridium difficile infections typically recover within two weeks of starting antibiotic treatment. However, many people become reinfected and need additional therapy. Most recurrences happen one to three weeks after stopping antibiotic therapy, although some occur as long as two or three months later.
Should you take probiotics if you have C. diff?
Clinicians are finding that there really is no basis to recommend probiotics for patients with Clostridioides difficile infection, that instead they may cause harm, said Colleen R. Kelly, MD, FACG, gastroenterologist and associate professor of medicine at The Warren Alpert Medical School of Brown University.
What is the most promising treatment for C difficile infection?
Metronidazole and oral route vancomycin have been the gold standard in treatment of C. difficile-associated diarrhea. Relapse rates of C. difficile have been noted as high as 20% to 30%, causing a search for the most superior agent for the treatment of this infectious disease.
Can Keflex cause C. diff?
Cephalexin, like almost all antibiotics, may cause mild or severe cases of pseudomembranous colitis, a mild to severe inflammation of the colon. Antibiotics, including cephalexin alter the types of bacteria in the colon and permit overgrowth of a bacterium called Clostridium difficile (C. diff.).
Can ceftriaxone cause C. diff?
Ceftriaxone is one of the cephalosporins most commonly associated with C. difficile infection. This is thought to be related to high rates of biliary excretion, which produces high concentrations of ceftriaxone in the gut [28].
Can Zpack cause C. diff?
Azithromycin and other macrolide antibiotics are considered to have a moderate risk of causing or contributing to C. difficile infections. Medical professionals have suggested substituting tetracyclines for macrolides when treating some conditions in older patients who are at greater risk of C.
What are the side effects of doxycycline?
Advertisement
- Blistering, peeling, or loosening of the skin.
- decreased appetite.
- diarrhea, watery and severe, which may also be bloody.
- difficulty with swallowing.
- feeling of discomfort.
- headache.
- hives, itching, puffiness or swelling of the eyelids or around the eyes, face, lips, or tongue.
- hives or welts, itching, or rash.
Can prednisone cause C. diff?
Among the drugs typically used to treat IBD, corticosteroids are perhaps the most powerful in terms of increasing risk for C difficile infection. Administrative data have suggested that corticosteroid exposure for any dose or duration significantly increases the risk of C difficile infection.